MERCURY: THE QUINTESSENTIAL ANTI-NUTRIENT
by Sara Russell, PhD, NTP, and Kristin G. Homme, PE(ret.), MPP, MPH
Townsend Letter January 2017
Comments by Ronald Peters, MD
This is an important review article which shows how mercury can devastate the body due to increased oxidative stress, enzyme inhibition, impaired cellular energy (ATP) production, cell wall dysfunction. These conditions are common to many patients and include the following:
- Impaired digestion with reduced stomach acid production,
- Increased sympathetic (fight/flight) nervous system tone,
- mitochondrial dysfunction with low energy production and fatigue,
- damage to the blood-brain barrier,
- increased bowel wall permeability and delayed onset food allergies,
- reduced immunity and allergies,
- autoimmunity,
- susceptibility to chronic infections such as Lyme and Candida,
- overloaded and impaired detoxification,
- multiple chemical sensitivities,
- chronic metabolic stress that creates adrenal fatigue,
- blood sugar problems and insulin resistance by blocking the insulin receptors,
- increasing fat storage and weight gain,
- stress intolerance,
- hypoglycemic symptoms due to impaired enzymes within the brain and/or HPA axis,
- oxidized blood vessels and cholesterol leading to arterial plaque,
- increased thrombosis and endothelial dysfunction in blood vessels,
- high or low blood pressure depending on whether artery calcification or artery deterioration and HPA dysfunction predominate,
- a type of heart failure due to mercury accumulation in the myocardium
Summary
 The chronic effects of cumulative, low-dose mercury exposure are underrecognized by both mainstream and alternative health authorities and, consequently, by the public. Mercury can cause or contribute to most chronic illnesses, including neurological disorders, cardiovascular disease, metabolic syndrome, chronic fatigue, fibromyalgia, adrenal and thyroid problems, autoimmunity, digestive disorders, allergies, chemical sensitivities, mental illness, sleep disorders, and chronic infections such as Lyme and Candida. Mercury toxicity should be suspected in individuals experiencing multiple health problems.
The chronic effects of cumulative, low-dose mercury exposure are underrecognized by both mainstream and alternative health authorities and, consequently, by the public. Mercury can cause or contribute to most chronic illnesses, including neurological disorders, cardiovascular disease, metabolic syndrome, chronic fatigue, fibromyalgia, adrenal and thyroid problems, autoimmunity, digestive disorders, allergies, chemical sensitivities, mental illness, sleep disorders, and chronic infections such as Lyme and Candida. Mercury toxicity should be suspected in individuals experiencing multiple health problems.- Diagnosis of chronic mercury toxicity is often difficult because the body’s natural defenses may mask or delay symptoms. Natural defenses are a function of genetic susceptibility, epigenetic factors, micronutrient status, and allostatic load (cumulative wear and tear on the body). Furthermore, individuals who retain mercury may counterintuitively show low levels in blood, urine, and hair.
- The developmental window from conception through early childhood is one of extreme vulnerability to mercury. Mercury is an epigenetic toxicant (affecting future gene expression) as well as a neurotoxicant. Damage may be permanent; therefore, prevention is key.
- For most people mercury is the most significant toxicant in the body. By promoting oxidative stress and depleting antioxidant defenses, including the glutathione system, mercury impairs the body’s response to toxicants in general including mercury itself.
- Mercury toxicity creates a need for extra nutrition, both to repair damage and to provide ample enzyme cofactors that can push blocked enzymes. Carbohydrate intolerance can be a symptom of mercury toxicity, and fat can be a preferred fuel. Many people with chronic mercury toxicity have found a nutrient-dense diet to be a useful starting point for symptom relief. Individualized supplementation may also be helpful to overcome the extreme nutritional depletion and unnatural toxic state.
Introduction
Mercury is an unusually insidious toxicant that can cause or contribute to most chronic illnesses. Its effects on various body systems can be mutually reinforcing, setting up a complex process of damage and dysfunction. For example, by inhibiting the glutathione system, which is key to detoxification, mercury perpetuates a vicious cycle of susceptibility and toxicity. As a result, mercury promotes nutritional depletion, oxidative stress, hormonal disruption, immune alteration, and neurotransmitter disturbances, which in turn can cause poor digestion, leaky gut, food allergies, altered gut flora, and autoimmunity. Yet, despite its pervasive ability to damage the body, mercury easily eludes detection; and many affected individuals have no idea that their unexplained health problems are due to past or ongoing mercury exposures.
Adding to the confusion, symptoms may manifest differently in each person depending on exposures, lifestyle, genetics, and micronutrient status. For example, it may manifest in one person as autoimmune issues such as Hashimoto’s thyroiditis, multiple sclerosis, or systemic lupus erythematosus and in someone else as mood, behavior, learning, or psychiatric problems. Long latencies may occur with onset of symptoms sometimes occurring months or years after the exposure has ceased.1,2 Many symptoms are vague, resembling premature cellular aging. Other symptoms are more distinct, a case in point being erethism (a constellation of personality traits including timidity, diffidence, contentiousness, insecurity, bluntness, rigidity, excitability, and hypersensitivity to criticism and to sensory stimulation).3-5 The term erethism, or reddening, derives from the person’s tendency to blush.6 Considering the subtle but reproducible effects of mercury on emotions, a number of problems that are blamed on character, personality, and stress may in fact be caused or compounded by low-level mercury toxicity.
Unfortunately, the public receives mixed messages from health authorities and agencies about the risks of mercury from routine exposures involving dentistry, fish, and vaccines. Certain exposure risks are widely discounted by the mainstream; yet according to the US Environmental Protection Agency, approximately 2–7% of women of childbearing age in the US have blood mercury levels of concern.7 And there is reason to believe that these regulatory levels of concern are too lax.i,8 In fact, neurodevelopmental disorders affect almost 11% of all US births, up 30% over the past decade;9 and subclinical decrements in brain function are even more common, affecting up to 15% of births.10 However, health authorities are unlikely to provide useful guidance on mercury risks for several reasons. Mercury is technically and politically difficult to study; thus, scientific conclusions about risks remain couched in uncertainty. Mercury’s effects are non-specific and multi-factorial. Finally, much exposure is iatrogenic – caused by health care – making it an unpopular topic.
Exposures
For most people, the major sources of mercury exposure are elemental mercury vapor from dental amalgams and methylmercury from dietary fish. Ethylmercury in certain vaccines provides smaller amounts, but these can be highly toxic during the vulnerable window of gestation and early childhood. These three forms of mercury are all easily absorbed and readily distributed throughout the body. Being lipophilic, these forms of mercury leave the bloodstream quickly, passing through biological membranes and concentrating in cells (including brain cells).11Mercury is especially drawn to high-sulfur organelles such as mitochondria. Once inside a cell, mercury is soon oxidized to Hg2+. This is a hydrophilic (lipophobic) form of mercury and therefore cannot easily pass through biological membranes. This form of mercury thus becomes trapped inside the cells, causing ongoing damage.12 Mercury has a particular affinity for the brain, where it may be retained indefinitely.13,14 It also accumulates in epithelial tissues, organs, and glands such as the salivary glands, thyroid, liver, pancreas, testicles, prostate, sweat glands, and kidneys as well as the epithelium of the intestinal tract and skin.15
| Table I: Common Exposures to Mercury
Dental amalgams – a few micrograms of mercury vapor per filling per day. |
Dental Amalgam
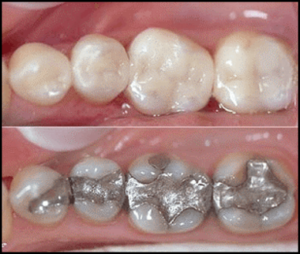 Dental amalgam, the material used in “silver fillings” beginning in the nineteenth century, is about 50% mercury. Mercury is highly volatile; consequently, amalgams continuously off-gas in the mouth. Health authorities have deemed amalgam as safe based on studies that were designed to detect only obvious harm, not subtle or long-term effects. New evidence indicates that susceptibility (and resistance) to mercury toxicity is driven by genes, only a few of which have been identified.16 Furthermore, evidence indicates that exposure from amalgams is sufficient to cause harm to susceptible people.17 The authors of the mercury chapter in the most recent metals toxicology textbook estimate that roughly 1% of the population is incurring clinical illness from their dental amalgams – and this is likely to be a gross underestimate because it excludes cases that have another diagnosis such as multiple sclerosis that may have a mercury component.18
Dental amalgam, the material used in “silver fillings” beginning in the nineteenth century, is about 50% mercury. Mercury is highly volatile; consequently, amalgams continuously off-gas in the mouth. Health authorities have deemed amalgam as safe based on studies that were designed to detect only obvious harm, not subtle or long-term effects. New evidence indicates that susceptibility (and resistance) to mercury toxicity is driven by genes, only a few of which have been identified.16 Furthermore, evidence indicates that exposure from amalgams is sufficient to cause harm to susceptible people.17 The authors of the mercury chapter in the most recent metals toxicology textbook estimate that roughly 1% of the population is incurring clinical illness from their dental amalgams – and this is likely to be a gross underestimate because it excludes cases that have another diagnosis such as multiple sclerosis that may have a mercury component.18
The World Health Organization estimates that the typical absorbed dose of mercury from amalgams is 1–22 micrograms per day with most values in the range of 1–5 micrograms per day.19Various factors including gum chewing and bruxism can increase these exposures to an upper range of about 100 micrograms per day.20 Preliminary evidence suggests that certain types of electromagnetic radiation including from mobile phones and from magnetic resonance imaging (MRI) may increase the release of mercury vapor from dental amalgams.21
In 2009, the US Food and Drug Administration (FDA) reiterated the safety of dental amalgam despite much scientific evidence to the contrary. As of 2016, public interest groups are challenging this “final amalgam rule” in federal court. Issues to be litigated include whether amalgam is deemed an implant, which would require manufacturers to provide proof of safety, and whether the toxicity warnings that are given to dentists via labeling requirements should also be given to patients. Norway, Denmark, and Sweden have banned dental amalgam; and, as of May 2015, a scientific committee of the European Commission recommends that non-mercury alternatives be used in fillings for pregnant women and children.22
As if the cumulative effects of ongoing amalgam exposure were not enough, unsafe amalgam removal can cause acute exposures to mercury vapor. Thus, patients wishing to replace amalgam fillings with less toxic alternatives must evaluate dentists’ use of adequate protective measures. The International Academy of Oral Medicine and Toxicology (IAOMT), a professional dental organization, has developed a protocol and training program that attempts to minimize the exposure to mercury vapor to the patient, dentist, and staff during amalgam removal. In women of childbearing age, removal of amalgam should be timed to avoid the 12–18 months preceding conception as a well as pregnancy and breastfeeding.
Dietary Fish
Mercury released into the atmosphere through natural and human activities is deposited in soil and water where it enters the food chain. Mercury accumulates in fish, particularly large, long-lived ocean fish. Natural releases from the Earth’s crust and the oceans account for 60–70% of the annual releases of mercury to the atmosphere. The remaining 30–40% is attributable to human activities.23 Thus, humans have always encountered some mercury in certain fish; and, as long as the natural defense systems are working, one can consume mercury-containing fish in moderation. In healthy individuals, intestinal metallothioneins (a class of metal-storage molecules that can be cumulatively damaged by mercury) can sequester ingested mercury and slowly allow its excretion. Selenium, discussed below, is a micronutrient that offers some protection against mercury and is found in fish as well as other foods.
Mercury levels in fish vary widely by species and by individual, ranging from less than 0.1 part per million (ppm) for salmon and sardines to more than 1 ppm for some samples of tilefish, shark, swordfish, and king mackerel. This means that a typical 3.5-ounce (100 gram) serving of fish could contain anywhere from a few micrograms to more than 100 micrograms of mercury. Tuna contains moderate levels, which vary by species. The FDA sets an Action Level for mercury contamination in commercial fish of 1.0 ppm; this means that federal officials are allowed to confiscate the product but not that they actually do so.
Vaccines
One of the most controversial aspects surrounding vaccines is their mercury content. Prior to about 2004, many childhood vaccines contained thimerosal, a preservative and adjuvant that is 50% ethylmercury.ii Childhood exposure to thimerosal rose sharply in the US during the 1990s as new vaccines were added to the childhood vaccine schedule set by the US Centers for Disease Control and Prevention (CDC). Infants subjected to the CDC vaccine schedule during this time typically received up to 187.5 micrograms of mercury in the first six months of life.24
No regulatory safety standard exists for ethylmercury. Because ethylmercury is chemically similar to methylmercury, the above-mentioned 187.5-microgram dose can be compared to the safe reference dose for methylmercury (the form present in dietary fish) set by the US Environmental Protection Agency (EPA) of 0.1 microgram per kilogram of body weight per day for chronic exposure, equivalent to about 0.3 micrograms per day for a newborn, and 0.6 micrograms per day for a 6-month old baby. Even if the 187.5-microgram exposure, delivered in a number of concentrated doses, is averaged over the six-month period, the resulting dose of 1.04 micrograms per day is still significantly higher than the EPA’s safe reference dose of 0.3–0.6 micrograms total per day for methylmercury. In addition, the EPA safe reference dose for methylmercury may be too lax,25,26 especially when applied to ethylmercury. Indeed, there may be no threshold that precludes adverse neuropsychological effects in children,27,28 whose brains are rapidly developing. Furthermore, unlike methylmercury from ingested fish, injected ethylmercury is not subject to the natural defense mechanisms related to ingestion, including metallothioneins and selenium, discussed later.
In 1999, the US Public Health Service called for the elimination of thimerosal from childhood vaccines. Nonetheless, due to supply and demand issues, it took several years to transition to reduced-thimerosal and then thimerosal-free alternatives.29
Additionally, during the period in which thimerosal began to be phased out of pediatric vaccines, the thimerosal-containing influenza vaccine became an important exposure source for fetuses and children. In 2002, the CDC began recommending that the influenza vaccine be given to children aged 6-23 months, as well as pregnant women in their second and third trimester, even though the only vaccine approved for these groups at the time was preserved with thimerosal.30 Furthermore, the CDC aggressively increased the dosing and expanded the target groups for the influenza vaccine, recommending a double dose for infants at both 6 and 7 months plus subsequent annual doses and a dose for all pregnant women, no longer limited as they previously had been to the second and third trimester.31 As of 2013, more than half of influenza vaccines were still preserved with thimerosal,32 with the availability of non-thimerosal versions subject to supply-and-demand dynamics. For example, the thimerosal-free flu vaccine shortage during the 2015 flu season led California’s governor to sign an exception allowing thimerosal-containing vaccines to be administered to infants and children despite a previous statewide restriction.
Some multi-dose meningococcal meningitis vaccines and tetanus toxoid (booster) vaccines (not recommended for children under six years of age), like the multi-dose influenza vaccines, also contain thimerosal as a preservative in amounts ranging from 12.5 to 25 micrograms per dose.33As of 2016, some childhood vaccine preparations still utilize thimerosal. In these vaccines, such as the multi-dose DTaP and the DTaP/Hib combination vaccines, most of the thimerosal is then filtered out, reducing thimerosal to “trace” amounts, according to the CDC.34
Other Exposures
Up to the early 2000s, broken mercury thermometers were a common exposure risk in many countries. Until the 1960s, teething powders for babies contained mercury in the form of calomel. Thimerosal was used in contact lens solutions. Merbromin was once widely used as an antiseptic under the trade name Mercurochrome. In 1998, such products were banned when the FDA declared that mercury as an active ingredient in over-the-counter products was not “generally recognized as safe (GRAS).” Nevertheless, the use of mercury as an inactive ingredient is allowed by the FDA provided its content is under 65 ppm, and FDA regulations regarding cosmetics do not obligate ingredients that make up less than 1% of the product to be disclosed on the label. For instance, some brands of mascara still contain thimerosal as an antimicrobial and preservative.
Compact fluorescent lamps (CFLs) typically contain about 4 milligrams (4,000 micrograms) of mercury, some of which is released upon breakage in the form of mercury vapor. The concentration of this toxic release is compared to various regulatory safety standards in Table II. CFL proponents argue that the energy savings offered by CFLs, which includes reduced mercury emissions from coal power plants, makes them desirable; but this debate is beyond the scope of this article.
Incinerators, coal-fired power plants, crematoria, and other industrial processes may be significant sources of local exposures to mercury. For over a decade, the EPA has attempted to restrict mercury emissions from coal plants in the US by about 90%; but the rule is under litigation, and legal experts predict that enforcement is years away.
In some countries, gold mining techniques that employ mercury (which were historically employed in the US during the Gold Rush) remain a significant source of exposure for miners and local populations.
Fetal and Childhood Exposures
Fetal neurons are more sensitive to the toxic effects of mercury than any other cell type.35Mercury from the mother’s body readily crosses the placenta and accumulates in the fetus, as revealed in post-mortem human and animal studies.36 In tissue culture, clear effects on nerve growth arise at mercury concentrations equivalent to those found in newborns of amalgam-bearing mothers with no other known exposures.37 Furthermore, mercury levels in amniotic fluid, cord blood, placental tissue, and breast milk are significantly associated in a dose-dependent manner with the number of maternal dental amalgam fillings.38,39 Human and animal studies show increased rates of miscarriage, neonatal death, low birth weight, and developmental disorders associated with mercury exposure.40
Developmental and Epigenetic Toxicity
The developmental period spanning from conception through early childhood is a window of vulnerability in which both epigenetic and neurological damage can occur at exposures far lower than those known to cause toxicity in adults. Epigenetics refers to the alteration of gene expression (turning genes on and off), usually via environmental factors, in a manner that can be passed to offspring without alteration of the DNA nucleotide sequence itself. Mercury is a potent epigenetic toxicant of alarming scope with both direct and indirect effects on gene expression. Mercury directly targets the cysteine that comprises the DNA-binding sites on most gene transcription factors. In addition, it targets the cysteine in DNA methyltransferase enzymes, which play a role (DNA methylation) in normal gene expression. Indirectly, mercury promotes severe oxidative stress – and early-life stressors are known to induce changes in gene expression that set the stage for disease in later life.41 Thus, unfortunately, when either parent is exposed to mercury, even prior to conception, the child’s own genetic expression can be affected.
Such epigenetic damage may range from mild to severe, and the resulting phenotype may include characteristics such as dental deformities, myopia, asymmetries of the face, and disproportions of the body. Such characteristics are described in Weston A. Price’s pioneering Nutrition and Physical Degeneration,42 whose ideas have subsequently been developed in Chris Masterjohn’s research on fat-soluble vitamins; in Sally Fallon Morell and Thomas Cowan’s Nourishing Traditions Book of Baby and Child Care43; and in the more epigenetically-focused Deep Nutrition by Catherine and Luke Shanahan.44Within the alternative health community, the role of micronutrients is well recognized to promote physical and mental health as well as optimal child development. Less well recognized is the role of toxicity in depleting one’s micronutrient status and the analogous role of micronutrient status in exacerbating or alleviating toxicities.
Genetic Susceptibilities
A loose scientific consensus has long discounted the idea of mercury toxicity from dental amalgams because population studies have shown that people with high exposures and even people with a high body burden do not necessarily have toxicity symptoms. Therefore, those who blame amalgams for their illnesses have been viewed askance. But within the past ten years, over a dozen common genetic variants that convey increased susceptibility to mercury toxicity have been documented in human studies.45,46 Moreover, hundreds more variants are likely to exist. Mercury attacks sulfur in proteins; and since the body has tens of thousands of genetically determined sulfur-containing proteins, many of these proteins are likely to include variants that contribute to susceptibility.47 Candidate genes are involved not only in methylation and detoxification but in vitamin and mineral (i.e., enzyme cofactor) absorption, transport, and metabolism. Yet genetic susceptibilities have yet to be considered by policy makers, health authorities, or the dental industry. Indeed, for millions of children and adults covered by subsidized dental programs, military family dental care, and Native American services, for example, amalgam is virtually the only option for dental restorations.
Regarding genetic susceptibilities to vaccine injury, a few isolated court cases in the US and elsewhere have recognized post facto that a limited number of well-documented genetic susceptibilities including some mitochondrial disorders have caused certain children to suffer permanent neurological damage. But genetic susceptibilities are a continuum, and the growing movement to mandate vaccines has so far failed to recognize this complex reality.
Mercury as Anti-Nutrient
Mercury’s toxicity is uniquely far-reaching. It disrupts fundamental biochemical processes, promotes oxidative stress, depletes antioxidant defenses, and destroys biological barriers. It causes numerous interacting effects across multiple organ systems,48 leading to a gamut of health issues ranging from fatigue and inflammation to endocrine and immune dysregulation and mood disorders.
Mercury readily binds to sulfhydryl (-S-H), a type of sulfur also called a thiol. The thiol is the major reactive site within the amino acid, cysteine, which is ubiquitous in biochemically active proteins such as enzymes. The human body contains tens of thousands of enzymes, which drive most fundamental biological processes. Mercury also binds strongly to selenium, a cofactor for several dozen enzymes involved in vital tasks such as thyroid function and brain antioxidant protection. Selenium is said to protect against mercury toxicity, but its protective scope is limited by its intracellular availability. This is governed by kidney processes that limit the amount of such minerals in the bloodstream and by specialized channels within the cell membrane that control mineral transport from the bloodstream into cells. Lipophilic mercury, on the other hand, has no such limits when entering cells. Moreover, selenoprotein P, a substance that stores and transports selenium to cells,49 can become blocked by mercury. Therefore, selenium offers only limited protection against mercury exposure.
The body’s most important intracellular antioxidant mechanism is the glutathione system. Because the glutathione molecule and its related enzymes employ cysteine, they are targets for mercury. Specifically, mercury damages the body’s glutathione system both by depleting the glutathione molecule itself and by blocking the enzymes that synthesize and recycle glutathione and facilitate its use. Glutathione detoxifies mercury by binding it (in a process called glutathione conjugation) into a less toxic form suitable for excretion through the bile. Incidentally, the glutathione system has been found to be crucial in the detoxification of thimerosal.50 By depleting glutathione and disabling the glutathione-related enzymes, mercury impairs the detoxification of many toxicants, including mercury itself, leading to increased toxicity.
By damaging methylation enzymes, including methionine synthase, mercury dysregulates the methylation cycle, a biochemical pathway in which the sulfur-containing amino acid methionine is recycled, creating two important products: s-adenosyl methionine (SAMe), the body’s universal methylator; and cysteine, the precursor for the transsulfuration pathway, which in turn produces glutathione, sulfate, and taurine. By impairing the methionine synthase enzyme, mercury blocks not only detoxification via the transsulfuration pathway that produces glutathione but also the production of many hormones and neurotransmitters that require methyl donors like SAMe. A lack of methyl donors also inhibits the activity of the DNA methyltransferase enzymes, which regulate gene expression.
In addition to attacking the sulfur in enzymes, mercury attacks the sulfur in the functional proteins within cell membranes. These include membrane transport channels that allow micronutrients into cells. One result, for example, is altered homeostasis of many essential minerals, which can appear abnormally high or low on testing and is an aspect of many chronic illnesses that has no other obvious explanation. Additionally, mercury may target the disulfide bonds in collagen, the connective tissue found in blood vessels, in the gut, and throughout the body. More importantly, mercury impairs the ongoing synthesis and repair of collagen, bone, and cartilage, both by impairing the necessary enzymes and by depleting a required cofactor – vitamin C. Thus mercury can be implicated in arthritis, osteoporosis, and connective tissue disorders.
Mercury promotes oxidative stress in several mutually reinforcing ways. Within cells, mercury concentrates in mitochondria, the organelles that synthesize ATP energy. There, it displaces iron and copper, converting them to free radicals with the potential to cause ongoing oxidative stress unless buffered by antioxidants. Mercury also blocks mitochondrial enzymes, creating an overproduction of reactive oxygen species, including free radicals. The resulting oxidative stress further damages mitochondrial enzymes as well as harming mitochondrial membranes and mitochondrial DNA. Mitochondrial dysfunction can result in overproduction of lactic acid, yielding metabolic acidosis, which depletes minerals and may promote certain pathogens. Mitochondrial damage further drains cellular energy by creating a disproportionate need for repair, perpetuating a vicious cycle.51 Mitochondrial dysfunction affects immunity, digestion, cognition, and any energy-intensive system within the body and is a key component of many chronic illnesses.
Oxidative stress perpetuates another vicious cycle in which free radicals cause lipid peroxidation, a self-propagating chain reaction in which the unsaturated fatty acids in cell membranes are attacked, becoming free radicals themselves, and ultimately leading to excess permeability in membranes and other barriers, thus provoking still more damage.
Metallothioneins are cysteine-rich metal storage molecules that appear to play a role in storing zinc and copper and are found in high levels in the intestines. When metallothioneins become saturated with mercury, they can no longer store zinc or copper or protect the body from mercury. It is much more common for mercury-affected people to suffer from low zinc than from low copper for several reasons. Dietary sources of zinc are more limited than for copper. Excess copper is excreted into the bile and removed from the body via the feces, but many people have sluggish bile flow and/or constipation, causing copper to accumulate in the liver. Additionally, estrogen dominance, which may be amplified in mercury-affected individuals due to common hormonal imbalances, causes copper retention. Estrogen dominance is common, especially in women, due to exposure to plastics, soy, flax, and other estrogenic foods as well as hormonal birth control products. Copper pipes, copper IUDs, and copper sulfate sprayed on crops as an anti-fungal (even on many organic crops) add to the overall copper load. Because copper and zinc are antagonistic, the more that copper is retained by the body, the more that zinc tends to be depleted.
Mercury-induced anomalies in the transport of essential minerals such as magnesium and zinc cause an extra need for these minerals in the diet. Furthermore, many health conditions caused by mercury toxicity are aggravated by low magnesium and/or zinc including cardiovascular disease, fibromyalgia, autism spectrum disorders, attention deficits, and depression. Not every person with a history of mercury exposure is deficient in all of these nutrients, however; and it is important to note that minerals have complex synergistic and antagonistic relationships. For example, low zinc is often accompanied by high copper, and low magnesium is often accompanied by high calcium in soft tissues.
Mercury’s toxicity may be amplified by exposure to other toxic metals, including lead, cadmium, and aluminum. Mercury and lead, in particular, are highly synergistic. In fact, in one study, a dose of mercury sufficient to kill 1% of the lab rats (lethal dose “LD01”) when combined with a dose of lead sufficient to kill 1% of the rats resulted in killing 100% of the rats.52 A similar test involving mercury and aluminum in cultured neurons killed 60% of the cells when the two low-dose toxicants (LD01) were combined.53 Even antibiotics have been shown to enhance the uptake, retention, and toxicity of mercury.54 Additionally, testosterone appears to aggravate mercury toxicity during development while estrogen protects against it.55 In fact, more boys than girls are diagnosed with autism spectrum disorders and attention deficit.
Autism, Attention Deficit and Other Neurological Disorders
Many scientific studies suggest a connection between mercury and autism spectrum disorder (ASD), yet the subset of studies cited by health authorities fails to find a causal link.56 Such a link is widely viewed as biologically plausible,57 yet remains a taboo subject in mainstream medicine and the media. Autism is documented to involve oxidative stress, mitochondrial dysfunction, immune or inflammatory processes, impaired sensory processing, and abnormal mineral homeostasis, all of which are consistent with mercury toxicity.58 Autistic children have been found to have significantly higher exposure to mercury during fetal development and early infancy, as measured by metals in baby teeth.59 The element most frequently deficient in ASD is zinc.60 Other commonly observed mineral imbalances in ASD include low calcium, iron, magnesium, manganese, and selenium as well as high copper and elevated toxic metals, which can sometimes be difficult to detect through testing, as described later.
Attention deficit disorder (ADD) and attention deficit hyperactivity disorder (ADHD) are common early findings in mercury-exposed children.61 Zinc deficiency has been identified as a biomarker for ADHD62; and the abnormal mineral profile for ADHD appears quite similar to that for autism and mood disorders, with the exception that ADHD typically includes iron overload. Additionally, copper dysregulation is a key factor in ADHD.63
Many studies report a close association between clinical depression and zinc deficiency with severity of symptoms inversely correlated with serum zinc levels. Decreased levels of zinc, calcium, iron, and selenium have been reported as risk factors for postpartum depression.64 Other neurological and psychiatric disorders associated with mercury include narcolepsy, obsessive-compulsive disorder, schizophrenia, bipolar disorder, Tourette syndrome, and borderline personality disorder as well as neurodegenerative disorders – Alzheimer’s, Parkinson’s and Multiple Sclerosis, for example. Each has been documented to involve oxidative stress, inflammation, mitochondrial dysfunction, and mineral imbalances; all of which can be attributed to mercury. These diseases are complex, such that human studies are unlikely to find a direct causal link with any one risk factor that is strong enough to satisfy skeptics; but a growing body of evidence suggests that mercury plays a major role.65
Exacerbating the mineral dysregulation associated with these many conditions are the neurotransmitter imbalances provoked by mercury. For example, mercury increases extracellular levels of the excitatory neurotransmitter glutamate, thus overactivating glutamate receptors on cell surfaces.66 The amplification of glutamate is further exacerbated by mercury’s inhibition of the calming neurotransmitter GABA67: Mercury blocks GABA receptors; it disproportionately destroys GABA-producing Purkinje neurons; and it impairs glutamate decarboxylase (GAD), the enzyme responsible for converting glutamate to GABA. Furthermore, mercury’s dysregulation of glutamate and GABA is associated with depression and suicide.68-70
Altered Microbiota, Digestive Dysfunction and Immune Health
Mercury is known to alter the intestinal microbiota, yielding increased levels of undesirable mercury-resistant bacterial species, which may also develop resistance to antibiotics.71-73 For example, the opportunistic yeast Candida albicans may overgrow, causing a host of unpleasant symptoms. This dysbiosis may be exacerbated by mercury’s dysregulation of the immune system as well as its promotion of metabolic acidosis. All this has negative implications for digestion, immunity, and mental health.74-76
Mercury also inhibits several enzymes affecting digestion including gastric hydrogen-potassium-ATPase, the enzyme that allows the synthesis of hydrochloric acid via the stomach’s proton pump. In addition, by promoting oxidative stress, mercury moves the autonomic nervous system into sympathetic (stress) mode, inhibiting digestion. Furthermore, the mitochondrial dysfunction from which many mercury-affected individuals suffer impairs digestion as well as other bodily functions. By damaging both the gut and the blood-brain barrier, mercury leads to leaky gut, which in turn leads to food allergies and brain disorders caused by maldigested proteins entering the bloodstream. As a fairly common case in point, partially digested proteins in foods containing gluten and casein may be metabolized into the opioid peptides gluteomorphin and casomorphin.77This is often seen in children with autism spectrum disorder and explains many parental reports of symptom relief on a gluten-free, casein-free diet.
Mercury’s effects on the gut can exacerbate mercury’s effects on the immune system. Mercury is known to cause allergies, reduced immunity, and autoimmunity78; and such immune dysfunction plays a role in many chronic illnesses. Reduced immunity yields susceptibility to chronic infections such as Lyme and Candida. Finally, although technically not an allergy, multiple chemical sensitivities can result from mercury overloading the body’s detoxification system and blocking metabolic enzymes in the liver and other tissues so that common but undesirable chemicals such as fragrances are metabolized incompletely, yielding toxic intermediates.
Thyroid Disorders, Hypothalamus-Pituitary-Adrenal Dysfunction, and Stress-Related Disorders
Mercury is known to concentrate in glands, including the thyroid and pituitary, and to impair the hypothalamus-pituitary-adrenal (HPA) axis. HPA function and thyroid function are tightly interrelated, with impairment of one system often causing impairment of the other. Mercury blocks the selenium-dependent enzyme that converts the thyroid hormone, thyroxine (T4), to its active form, triiodothyronine (T3). Unfortunately, despite symptoms, the resulting hypothyroidism often goes undetected by routine blood work, which typically only tests levels of TSH, the hormone secreted by the pituitary that signals the thyroid gland to produce T4. Further suppressing thyroid function is the mercury-induced depletion of selenium and zinc, which are cofactors for thyroid enzymes.
The oxidative stress caused by mercury is a type of chronic stress that depletes the HPA axis; thus, mercury is implicated in the cluster of symptoms referred to as adrenal fatigue. Incidentally, an evolving view of this condition suggests that it is not a glandular problem, but rather a brain-stress problem.79 Early-life exposure to mercury also causes epigenetic damage to the HPA axis, which can dysregulate the stress response throughout life. This may involve a tendency toward either high or low baseline cortisol as well as a loss of the dynamic cortisol response to stress.80 The latter yields a disabling feeling of unwellness and stress intolerance. High baseline cortisol, on the other hand, may feel less debilitating, but this is a catabolic state that can promote degeneration of otherwise healthy tissues.
Metabolic Disorders, Obesity, and Cardiovascular Disease
HPA dysregulation and thyroid dysfunction strongly impact metabolism and weight. As an epigenetic toxicant, mercury can cause a host of metabolic issues, including blood sugar problems, insulin resistance, and stress intolerance. These symptoms can persist throughout life and into future generations. In addition, mercury impairs many enzymes needed to metabolize food into energy including pyruvate dehydrogenase, which is required for metabolism of carbohydrates but not fat or proteins. Hypoglycemic symptoms, which are common in mercury toxicity, may not reflect true low blood sugar but may indicate impaired enzymes within the brain and/or HPA axis. Other enzymes impaired by mercury include those of the citric acid cycle and the electron transport chain, leading to low ATP energy. Mercury also blocks the insulin receptor, promoting high insulin and thus fat storage. Mercury can cause weight gain or weight loss, depending on whether metabolic dysregulation or gut dysfunction predominates.
Regarding mercury’s role in cardiovascular disease, mercury oxidizes blood vessels as well as cholesterol, leading to arterial plaque. Mercury promotes thrombosis and endothelial dysfunction in blood vessels.81 Mercury can cause high or low blood pressure depending on whether artery calcification or artery deterioration and HPA dysfunction predominate. Finally, in a remarkable example of how mercury accumulates in certain tissues, a biopsy study of 13 patients with a type of heart failure found that mercury levels in the myocardium were 22,000 times higher than normal.82
Nutrition
Mercury damage creates a need for extra nutrition, both to repair damage and to prod blocked enzymes. Nutrient-dense diets are of critical importance, and targeted supplementation may help to overcome the unnatural toxic state. Because everyone’s nutrient status is uniquely affected by mercury, it is wise to take an individual approach rather than supplement all potentially depleted nutrients across the board. In addition, dietary modifications are sometimes necessary to control the inflammation and other symptoms that result from food sensitivities, which are common in affected individuals. Also, eating foods to which we are allergic or intolerant impairs detoxification by placing undue stress on the organs of digestion and elimination, putting the HPA axis on alert, and increasing the level of inflammation in the body. It is common for people with mercury toxicity to have multiple food sensitivities, particularly to gluten, casein, and soy.
High-quality fat is a preferred fuel in mercury toxicity, because it supplies much-needed fat-soluble vitamins and helps stabilize blood sugar levels. Additionally, because both brain tissue and the phospholipid bilayer of the cell membrane are built in large part from saturated fat, consumption of grass-fed animal fats such as lard, tallow, ghee, and butter contributes to repair. Cod liver oil, liver, extra-virgin organic olive oil, red palm oil, and lard are important sources of fat-soluble vitamins; and it is important to eat a variety of healthy fats from both animal and plant sources. Fat metabolism requires fewer enzymes than carbohydrate metabolism, thus has less opportunity to be blocked by mercury. In addition to slowing energy production, impaired enzymes can create toxic intermediates, which can yield food intolerances to some carbohydrate foods. Carbohydrates can raise insulin, the fat-storage hormone, which may already be high due to mercury toxicity. Finally, high-carbohydrate foods are more likely than high-fat foods to contain anti-nutrients such as phytates, oxalates, and lectins.
Bone broth is ideal for repairing the digestive lining and connective tissue, and for supplying easily assimilated amino acids and other nutrients. Daily consumption of bone broth can help repair the excessive gut permeability that often leads mercury-toxic individuals to food allergies and autoimmunity. Glutamine is one of the most important amino acids needed to repair the lining of the gut; and glutamine and glycine, both abundant in bone broth, are precursors to the body’s production of glutathione. Vitamin B6 and magnesium may ease the conversion of glutamate to GABA.83 In the event of sensitivity to glutamate, it is advisable to simmer the broth for no longer than 3-4 hours.
Beet kvass can improve the flow of bile and thus improve excretion of mercury and other toxicants through the bile, particularly in individuals who tend to be constipated. Other probiotic foods, such as sauerkraut, are also helpful as part of a healing program. It is a good idea to start with a small amount of probiotic foods and to increase gradually as tolerated. Organ meats are nutrient-dense and can help supply vitamins and minerals depleted by mercury. For example, liver is high in vitamins A and B-12 as well as zinc, magnesium, and selenium.
Foods high in vitamins A, C, D and E confer important antioxidant and immune-modulating benefits. Vitamin C helps rebuild damaged collagen and can be obtained from a variety of food sources as tolerated, taking care not to rely entirely on the sweeter fruits, which can be problematic for people with blood sugar issues. Good sources of the vitamin include rose hips, guava, acerola cherry, lemons, limes, oranges, grapefruit, kale, broccoli, cauliflower, Brussels sprouts, papaya, mango, pineapple, kiwi, and strawberries. People who suffer from thiol sensitivity, discussed below, will need to avoid or limit the vegetables included on the list. Because grapefruit can stimulate phase II of the liver’s detoxification and slow down phase I, it is wise to consume grapefruit only occasionally unless phase I is already known to be overly active with respect to phase II.
The two minerals most commonly depleted by mercury are magnesium and zinc. Liver, leafy green vegetables, nettles, properly soaked lentils (if tolerated), and properly prepared almonds are good sources of magnesium. Nettles are a great source of numerous vitamins and minerals, including magnesium, and can be added to soups or enjoyed as a tea. Zinc-rich foods are critical, but unfortunately oysters, the richest source of zinc, also tend to be high in cadmium and other heavy metals. Thus, red meat and poultry, along with properly soaked sesame and pumpkin seeds and pine nuts, are important sources of zinc for mercury-affected people, keeping in mind that we absorb zinc much more efficiently from animal foods than from plant sources.
Brazil nuts are a good source of selenium, and, unlike fish that are also high in selenium, do not contain potentially problematic levels of mercury. The selenium content of Brazil nuts varies according to the soil where the nuts are grown, as is the case for all foods. Brazil nuts are high in unsaturated fat and may not keep well if soaked extensively, but overnight soaking works well in temperate climates. Regarding the consumption of fish, the evidence suggests that once the body’s natural defenses have been overrun by mercury the selenium in seafood is less effective in buffering the mercury. Thus, people who know or suspect a mercury problem must consider the benefits and the risks in determining their fish consumption level. For example, those who limit their seafood intake should consider taking cod liver oil and perhaps fish oil as well in order to derive some of the nutritional benefits of fish while keeping mercury exposure as low as possible.
Elimination and reintroduction of suspect foods is the best way to assess whether these foods are problematic for an individual. The goal is the least restrictive nutrient-dense diet. For example, many children and adults with mercury toxicity benefit from a gluten-free, casein-free diet while others can tolerate one or both of these foods. Additional intolerances too numerous to list affect certain mercury-toxic individuals to varying degrees. The intake of alcohol, sugar, refined starches, processed foods, caffeine, medications, etc. reduces the body’s ability to detoxify, causing unpleasant symptoms in many affected individuals. Additionally, the common intolerance to sulfites in wine suggests impairment of the sulfite oxidase enzyme needed to convert toxic sulfite to beneficial sulfate. This enzyme can be boosted by supplementing its cofactor, molybdenum. Also, because mercury blocks metabolic enzymes such as phenolsulfotransferases, certain food compounds, such as phenols, become partially metabolized into toxic intermediates, often resulting in reactions such as red cheeks and/or ears and hyperactivity after consuming foods high in phenol.84 Additionally, yeast overgrowth can increase sensitivity to high-thiol and high-oxalate foods.
Foods high in free thiols (which include legumes, dairy, the cabbage family, eggs) may be poorly tolerated by some mercury-affected individuals, particularly if the transsulfuration pathway is compromised, as can occur with molybdenum deficiency. Other sulfur-rich foods, such as red meat and organ meats, do not cause such problems. Of course it is important to consume a diet that includes all the essential amino acids, including those that contain sulfur. Andrew Cutler, author of Amalgam Illness: Diagnosis and Treatment (see Resources, below) and Hair Test Interpretation: Finding Hidden Toxicities notes that foods high in free thiol can provoke symptoms in a significant subset of mercury-affected people, in part by increasing plasma cysteine, which may rise in response to mercury and its biochemical effects. Vegetarian diets are particularly deleterious to a significant subset of people suffering from mercury toxicity because it is virtually impossible to obtain sufficient protein on a vegetarian diet that is modified to reduce free-thiol sources.
A problematic food for many mercury-toxic individuals is cilantro leaf, which contains a chelating substance capable of redistributing mercury, thus exacerbating symptoms in sensitive individuals. Unfortunately, within the alternative health community, cilantro leaf is sometimes recommended in large amounts in both food and supplement form. Also often recommended is chlorella, which is inadvisable as a supplement due to its potential for contamination from the environment in which it is grown and to its lipopolysaccharide content, which can cause inflammatory stress.85
Each mercury-toxic person has a unique combination of mineral imbalances that affect how mercury toxicity is expressed and what particular nutrient combination is likely to provide relief. Mineral dysregulation is significantly more pronounced in people with chronic mercury toxicity than in the general population,86 as are other nutritional deficiencies and food intolerances.
Testing
Testing for mercury toxicity is not straightforward. Mercury may accumulate in organs like the brain even while blood, urine, fecal and hair levels are low. Urine challenge tests should be avoided. They involve the administration of a chelator in a dosage high enough to cause significant oxidative stress due to redistribution of toxic metals to target organs such as the brain and kidneys. A porphyrin panel can reveal the footprint of toxic metals including mercury. Porphyrins are undesirable byproducts that occur when enzymes are blocked by toxicants. But since porphyrins are easily destroyed,87 the risk of false negatives is high unless the sample is handled carefully. A hair elements test can reveal apparent dysregulation of essential mineral homeostasis – i.e., essential hair minerals will appear abnormally high and/or low – and thus may serve as an economical screening test for chronic mercury toxicity. Note that when hair essential minerals are dysregulated, a high level of an essential mineral may not indicate adequate intracellular status but may simply mean high excretion in hair.
It is beyond the scope of this nutrition-focused article to discuss mercury treatment options, but we recommend caution when considering detoxification protocols. For the highly mercury toxic, many products may be either unsafe (such as chlorella and cilantro) or may be used in an unsafe manner (such as alpha lipoic acid). Alpha lipoic acid is added to many nutritional supplements without warning about its metal chelating properties. When taken by individuals who have mercury dental amalgams or a body burden of mercury, it can pull mercury from the teeth and other tissues in an attempt to equilibrate levels throughout the body and brain. This is especially tragic when fetal exposure is involved. We suggest that anyone wishing to deepen their knowledge of mercury detoxification read the books by Andrew Cutler listed in the Resources section. Cutler’s work is the most useful compilation of science-based explanations of mercury toxicity and its myriad effects. It should be noted that Cutler’s chelation protocol, though grounded in scientific theory, is controversial and is not without risk.
Conclusions
Because of mercury’s powerful anti-nutrient effects, a nutrient-dense diet may alleviate many symptoms of chronic mercury toxicity. Moreover, the nutritional depletion caused by mercury is so pervasive that affected individuals often require nutritional supplementation as well as a nutrient-dense diet. At the same time, it’s important to note that many mercury-affected individuals are quite sensitive to a large number of foods, supplements, and medications. Many people with a hidden mercury burden find relief by following a nutrient-dense diet, adapted as necessary to avoid gluten and/or dairy and to limit sugars and starches.
Mercury creates a biochemical train wreck in the body and has the toxic power to cause or contribute to most chronic illnesses. People who have multiple health problems may suffer from undiagnosed chronic mercury poisoning. Mercury depletes nutrients needed for vital functions and dysregulates mineral and neurotransmitter metabolism to a greater extent than any other common toxicant.
Yet chronic mercury toxicity remains underrecognized by both mainstream and alternative health authorities for a number of reasons. The scientific literature on mercury is complicated, incomplete, and easily misinterpreted. Mercury demonstrates a complex, nonlinear toxicity. Mercury susceptibility depends on genetics, epigenetics, and micronutrient status. The body’s natural defenses may mask toxicity, creating long latencies between exposures and symptoms. Symptoms are varied and nonspecific and may be intermittent in the early stages. Mercury research is controversial because much exposure has been iatrogenic, via dental amalgams and vaccine preservatives. Toxicity testing is not straightforward, as described above. In summary, the combination of ubiquitous exposures, iatrogenic involvement, long latencies, broad toxic effects, nonspecific symptoms, and potentially irreversible damage renders chronic mercury toxicity an underrecognized epidemic.
Resources
- IAOMT.org – International Academy of Oral Medicine and Toxicology, a professional dental association that provides fact sheets about mercury and describes the Academy’s safe amalgam removal protocol
- MercuryFreeBaby.org – a joint project of IAOMT and CoMeD (Coalition for Mercury-Free Drugs), which advocates removal of mercury from all vaccines
- Amalgam.org – Dental Amalgam Mercury Solutions, a non-profit organization dedicated to educating consumers about unhealthy dental practices
- Amalgam Illness: Diagnosis and Treatment (1999) by Andrew Hall Cutler. This book is still the most complete, science-based, self-help book on chronic mercury toxicity to date. Available through the author’s website at www.noamalgam.com as well as online bookstores: .
- Mercury Poisoning: The Undiagnosed Epidemic (2013) by David Hammond. This book provides more context and less physiology than Cutler’s book in a rendition some may find more readable.
- livingnetwork.co.za/chelationnetwork/food/high-sulfur-sulphur-food-list/ – a resource that explains why some people with mercury toxicity cannot tolerate thiols and how to identify thiol intolerance.
- http://www.ewg.org/skindeep/ – the Environmental Working Group’s Skin Deep® searchable online consumer database of body care products ranging from basics such as soap and shampoo to sunscreen and cosmetics.
Acknowledgements: The authors would like to thank Nori Hudson, NC,
Andrew Hall Cutler, PhD, PE, Janet Kern, PhD, Marco Prina, PhD, Rebecca
Rust Lee, and Lana Russell for their input and reading of the article at
various stages of its drafting and revision.
== ==
Mercury: The Quintessential Anti-Nutrient by Sara Russell, PhD, NTP, and
Kristin G. Homme, PE(ret.), MPP, MPH
References
Mutter J, Naumann J, Sadaghian C, Walach H, Drasch G. Amalgam studies: disregarding basic principles of mercury toxicity. Int J Hyg Environ Health. 2004;207:391–397.
- Weiss B, Clarkson TW, Simon W. Silent latency periods in methylmercury poisoning and in neurodegenerative disease. Environ Health Perspect. 2002;110 (Suppl 5):851–4.
- Waldron HA. Did the Mad Hatter have mercury poisoning? Br Med J.1983;287 (6409):1961.
- Grum, DK, Kobal AB, Arnerič _N, et al. Personality Traits in Miners with Past Occupational Elemental Mercury Exposure. Environ Health Perspect.2006;114(2):290-296.
- Clarkson, TW, Magos, L. The toxicology of mercury and its chemical compounds. Crit Rev Toxicol. 2006;36:609–662. Gerstner HB, Huff JE. Clinical toxicology of mercury. J Toxicol Environ Health. 1977;2(3):491–526.
- Mahaffey KR, Clickner RP, Jeffries RA. Adult women’s blood mercury concentrations vary regionally in the United States: association with patterns of fish consumption (NHANES 1999-2004). Environ Health Perspect. 2009;117(1):47-53.
- Gump BB, MacKenzie JA, Dumas AK, et al. Fish Consumption, Low-Level Mercury, Lipids, and Inflammatory Markers in Children. Environ Research.2012;112:204-211.
- Boyle CA, Boulet S, Schieve LA, et al. Trends in the prevalence of developmental disabilities in US children, 1997-2008. Pediatrics.2011;127(6):1034-42. The authors provide the following figures: ADHD + Autism + seizures + stutter = 7.57% + 0.74% + 0.72% + 1.68% = 10.71%. Grandjean P, Landrigan PJ. Neurobehavioural effects of developmental toxicity. Lancet Neurol. 2014;13(3):330–8.
- Berlin M, Zalups RK, Fowler BA. Mercury. In: Nordberg GF, Fowler BA, Nordberg M, eds. Handbook on the Toxicology of Metals. 4th ed. Amsterdam [etc.]: Elsevier/Academic Press; 2015. pp. 1013–75.
- Berlin Ibid.
- Berlin Ibid.
- Rooney JP. The retention time of inorganic mercury in the brain – a systematic review of the evidence. Toxicol Appl Pharmacol.2014;274(3):425-35.
- Berlin, et al. 2015, op. cit.
- Homme K, Kern JK, Haley B, et al. New Science Challenges Old Notion that Dental Amalgam is Safe. Biometals. 2014:27;19-24.
- Ibid.
- Berlin, et al. 2015, op. cit.
- IPCS (International Programme on Chemical Safety). Elemental mercury and inorganic mercury compounds: human health aspects. World Health Organization, United Nations Environment Programme; 2003. Accessed Dec. 29, 2015.
- Berlin et al. 2015, op. cit.
- Mortazavi G, Mortazavi SM. Increased mercury release from dental amalgam restorations after exposure to electromagnetic fields as a potential hazard for hypersensitive people and pregnant women. Rev Environ Health. 2015;30(4):287-92.
- EC European Commission Health and Food Safety Scientific Committee. Final opinion on dental amalgam. May 015.,http://ec.europa.eu/health/scientific_committees/consultations/public_consultations/scenihr_consultation_24_en.htm. 29 April 29, 2015. Accessed June 18, 2015.
- Berlin, et al. 2015, op cit.
- Geier DA, King PG, Hooker BS, et al. Thimerosal: Clinical, epidemiologic and biochemical studies. Clinica Chimica Acta. 2015;444:212–20.Rice DC. The US EPA reference dose for methylmercury: sources of uncertainty. Environ Res. 2004;95(3):406-13.
- Budtz-Jørgensen E, Grandjean P, Weihe P. Separation of risks and benefits of seafood intake. Environ Health Perspect. 2007;115(3):323-7.
- Rice 2004, op. cit.
- World Health Organization. Mercury in Health Care, Policy Paper. August 2005. http://www.who.int/water_sanitation_health/medicalwaste/mercurypolpaper.p Accessed April 28, 2016.Geier et al. 2015, op. cit.
- Ibid.
- Ibid.
- Ibid.
- See for example the FDA’s chart on “Vaccine Safety and Availability” at http://www.fda.gov/BiologicsBloodVaccines/SafetyAvailability/VaccineSafety/UCM096228#t1 and the National Vaccine Information Center (NVIC) Frequently Asked Questions on the topic of “Thimerosal in Vaccines” at http://www.nvic.org/faqs/mercury-thimerosal.aspx (both accessed Jan 12,2016).
- CDC brochure: Understanding Thimerosal, Mercury and Vaccine Safety. Revised 2013. http://www.cdc.gov/vaccines/hcp/patiented/conversations/downloads/vacsafe-thimerosal-color-office.pdf. Accessed January 12, 2016.
- Berlin et al. 2015 op. cit.
- Berlin Ibid.
- Ibid.
- Ibid.
- Kern JK, Geier DS, Bjørklund G, et al. Evidence supporting a link between dental amalgams and chronic illness, fatigue, depression, anxiety,and suicide. Neuroendocrinology Letters. 2014;35(7):537-52.
- Berlin et al. 2015, op. cit.
- Brigelius-Flohé R, Flohé L. Basic principles and emerging concepts in the redox control of transcription factors. Antioxid Redox Signal. 2011;15(8):2335–81.
- Price WA. Nutrition and Physical Degeneration (8th printing). Lemon Grove, CA: The Price-Pottenger Nutrition Foundation; 2011.
- Fallon Morell S, Cowan TS. The Nourishing Traditions Book of Baby and Child Care. Washington, DC: New Trends Publishing; 2013.
- Shanahan C and Shanahan H. Deep Nutrition: Why Your Genes Need Traditional Food. Lawai, HI, Big Box Books; 2008.
- Woods JS, Heyer NJ, Russo JE, Martin MD, Farin FM. Genetic polymorphisms affecting susceptibility to mercury neurotoxicity in children:summary findings from the Casa Pia Children’s Amalgam clinical trial. Neurotoxicology. 2014;44:288–302.
- Mutter et al. 2004, op. cit.
- Berlin et al. 2015, op. cit.
- Kern et al. 2014, op.cit.
- Burk RF, Hill KE. Selenoprotein P: an extracellular protein with unique physical characteristics and a role in selenium homeostasis. Annu Rev Nutr. 2005;25:215–35.
- Westphal GA, Schmuch A, Schulz TG, et al. Homozygous gene deletion of the glutathione S-transferases M1 and T1 as associated with thimerosal sensitization. Int Arch Occup Environ Health 2000;73(6): 384-88.
- Kern et al. 2014, op. cit.
- Schubert J, Riley EJ, Tyler SA. Combined effects in toxicology. A rapid systematic testing procedure: cadmium, mercury, and lead. Toxicol Environ Health. 1978;4(5/6):763-776.
- Haley BE. Mercury toxicity: Genetic susceptibility and synergistic effects. Medical Veritas. 2005:2;535–542.
- Ibid.
- Geier DA, Kern JK, Geier MR. The biological basis of autism spectrum disorders: Understanding causation and treatment by clinical geneticists. Acta Neurobiol Exp (Wars). 2010;70(2):209-26. Hooker B, Kern J, Geier D, et al. Methodological issues and evidence of malfeasance in research purporting to show thimerosal in vaccines is safe. Biomed Res Int. 2014.
- Berlin et al. 2015, op cit.
- Kern JK, Geier DA, Audhya T, King PG, Sykes LK, Geier MR. Evidence of parallels between mercury intoxication and the brain pathology in autism. Acta Neurobiol Exp (Wars). 2012;72(2):113–53.
- Adams JB, Romdalvik J, Ramanujam VM, Legator MS. Mercury, lead, and zinc in baby teeth of children with autism versus controls. J Toxicol Environ Health A. 2007;70(12):1046-51.
- Pfaender S, Grabrucker AM. Characterization of biometal profiles in neurological disorders. Metallomics. 2014;6(5):960–77. Woods et al. 2014, op cit.
- Pfaender S, Grabrucker AM. Characterization of biometal profiles in neurological disorders. Metallomics. 2014;6(5):960–77.Malter, Richard. The Strands of Health: A Guide to Understanding Hair Tissue Mineral Analysis. Cottonwood, AZ: Educational and Health Resources of Arizona, Inc.; 2002.
- Pfaender S, Grabrucker AM. Characterization of biometal profiles in neurological disorders. Metallomics. 2014;6(5):960–77.Carocci A, Rovito N, Sinicropi MS, Genchi G. Mercury toxicity and neurodegenerative effects. Rev Environ Contam Toxicol. 2014;229:1–18.
- Farina M, Avila DS, da Rocha JBT, Aschner M. Metals, oxidative stress and neurodegeneration: a focus on iron, manganese and mercury.Neurochem Int. 2013; 62(5):575–94.
- Kern et al. 2012, op. cit.
- Kern et al. 2014, op. cit.
- Sowa-Kućma M, Szewczyk B, Sadlik K, et al. Zinc, magnesium and NMDA receptor alterations in the hippocampus of suicide victims. J Affective Disord. 2013;151:924–931.
- Zarate C, Duman RS, Liu G, Sartori S, Quiroz J, Murck H. New paradigms for treatment-resistant depression. Ann N Y Acad Sci. 2013;1292:21–31.
- Kern et al. 2012, op. cit.
- Lorscheider FL, Vimy MJ, Summers AO, Zwiers H. The dental amalgam mercury controversy––inorganic mercury and the CNS; genetic linkage of mercury and antibiotic resistances in intestinal bacteria. Toxicology. 1995;97:19–22.
- Summers AO, Wireman J, Vimy MJ, et al. Mercury released from dental “silver” fillings provokes an increase in mercury- and antibiotic- resistant bacteria in oral and intestinal flora of primates. Antimicrob Agents Chemother. 1993;37:825–834.
- Diaz Heijtz R, Wang S, Anuar F, et al. Normal gut microbiota modulates brain development and behavior. Proc Natl Acad Sci USA. 2011;108:3047– 3052.
- Hansen CH, Nielsen DS, Kverka M, et al. Patterns of early gut colonization shape future immune responses of the host. PLOS One. 2012;7:e34043.
- Tlaskalová-Hogenová H, Stepánková R, Hudcovic T, et al. Commensal bacteria (normal microflora), mucosal immunity and chronic inflammatory and autoimmune diseases. Immunology Letters. 2004;93:97–108.
- Campbell-McBride N. Gut and Psychology Syndrome. Cambridge, MA: Medinform; 2010.
- Vas J, Monestier M. Immunology of mercury. Ann N Y Acad Sci. 2008;1143:240–267.
- Gedgaudas N, Kharrazian D. Rethinking Fatigue: What Your Adrenals Are Really Telling You and What You Can Do about It (ebook). Primal Body Primal Mind Publishing; 2014.
- Moisiadis VG, Matthews SG. Glucocorticoids and fetal programming part 1: Outcomes. Nat Rev Endocrinol. July 2014; 10(7):391–402.
- Houston MC. Role of mercury toxicity in hypertension, cardiovascular disease, and stroke. J Clin Hypertens (Greenwich). August 2011;13(8):621–7.
- Frustaci A, Magnavita N, Chimenti C, et al. Marked elevation of myocardial trace elements in idiopathic dilated cardiomyopathy compared with secondary cardiac dysfunction. J Am Coll Cardiol. 1999;33(6):1578-83.
- Cutler AH, Amalgam Illness: Diagnosis and Treatment. Sammamish, WA; 1999.
- Matthews J. Nourishing Hope for Autism: Nutrition and Diet Guide for Healing Children. 3rd Ed. Healthful Living Media; 2008.
- Hsu HY, Jeyashoke N , Yeh CH, Song YJ, Hua KF, Chao LK, Immunostimulatory bioactivity of algal polysaccharides from Chlorella pyrenoidosa activates macrophages via Toll-like receptor 4, J Agric Food Chem. 2010;58(2):927-36.
- Cutler, AH, Hair Test Interpretation: Finding Hidden Toxicities. Sammamish, WA; 2004.
- Woods JS. Urinary porphyrin profiles and genetic susceptibility to mercury toxicity. Presentation at the International Academy of Oral Medicine and Toxicology conference, San Antonio, Texas, March 2009. Available at http://www.youtube.com/watch?v=eW0kDV-jMF4.
Ready to Start?
Contact our team to schedule your next service!

